Hemostasis is the body's natural process for stopping bleeding, and it involves a complex series of steps. Here's what EMTs should know about the mechanism of hemostasis:
1. Vasoconstriction:
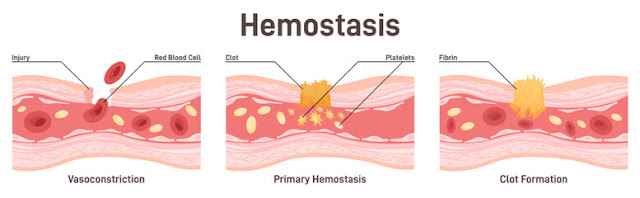
- When an injury occurs, the first response is vasoconstriction, which is the narrowing of blood vessels. This helps reduce blood flow to the injured area and minimizes the loss of blood.
- EMTs may observe vasoconstriction as part of the body's initial response to bleeding, with the skin around the wound appearing pale or blanched.
2. Primary Hemostasis:
- Primary hemostasis involves the formation of a platelet plug. Platelets are small cell fragments in the blood that adhere to the site of injury and to each other.
- Platelets become sticky in response to exposed collagen at the wound site. They adhere to the injured vessel wall and to each other to form a plug, temporarily sealing the breach in the blood vessel.
3. Secondary Hemostasis:
- Secondary hemostasis, also known as the coagulation cascade, is a series of complex reactions involving clotting factors that ultimately result in the formation of a stable blood clot.
- The coagulation cascade involves the conversion of fibrinogen into fibrin, which forms a mesh-like structure to reinforce the platelet plug and trap red blood cells to create a stable clot.
4. Clot Retraction and Repair:
- After the blood clot has formed, it undergoes retraction, which is the process of the clot contracting and pulling the edges of the wound together. This helps to limit bleeding.
- As the wound heals, tissue repair and regeneration occur to ultimately restore the integrity of the injured blood vessels.
5. Fibrinolysis:
- Once the injury is healed, the body initiates the process of fibrinolysis, which breaks down the fibrin clot. This is essential to prevent excessive clot formation and to restore normal blood flow.
In the pre-hospital setting, EMTs often intervene during primary hemostasis and secondary hemostasis to control bleeding. They can apply direct pressure, elevate the injured area, use hemostatic dressings, or apply tourniquets when necessary to help facilitate hemostasis.
Understanding the mechanism of hemostasis allows EMTs to make informed decisions about which techniques and interventions are most appropriate for each patient's specific bleeding situation.
Additionally, EMTs should be aware that certain medical conditions, medications, and coagulation disorders can affect the body's ability to achieve hemostasis, and they should take these factors into consideration when managing bleeding in trauma patients.
No comments:
Post a Comment